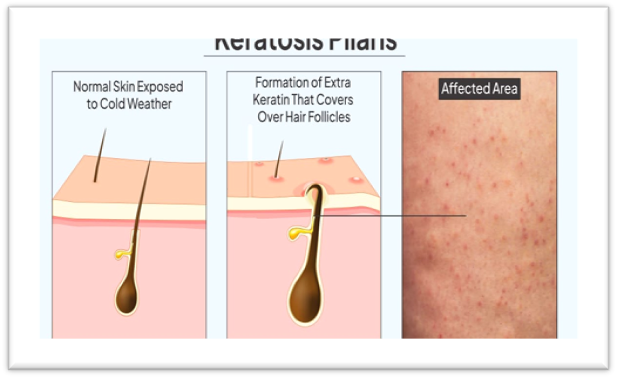
Keratosis pilaris often manifests in small, hard bumps on the legs and arms. A common treatment method for many acne conditions, such as keratosis pilaris, in such cases, mostly acids are used for the treatment, which have shown a promising effect in recent years. This review examines the use and success of multiple types of acids, steroids, and kinase inhibitors in clinical and non-clinical settings to treat and understand keratosis pilaris. In the treatment of keratosis pilaris, acid primarily works by breaking down the dead skin cells that clog the hair follicles. Some types of steroids have anti-inflammatory properties that have proven useful in minimizing the appearance of acne. Kinase inhibitors control important skin cell functions, such as cell signaling, metabolism, division, and survival, which undoubtedly affect the appearance of skin as a whole. The known impact of acid, steroids, and kinase inhibitors on keratosis pilaris is underestimated and should be given more attention by healthcare industry leaders.Further research is needed to better recognize the pathophysiology of Kertosis Pilaris and to discover more effective therapeutic interventions. Treatment options include topical exfoliants, moisturizers, and keratolytics, although Keratosis Pilaris typically resolves on its own over time. The condition is often mistaken for other dermatological issues, highlighting the need for accurate diagnosis and management.
Atopy, Coiled hair, Dermatological issues, Keratosis pilaris, Keratolytic, Topical exfoliants
CLINICAL FATURES:
Keratosis pilaris presents as small, rough, follicular papules, typically skin-coloured, red, or brown depending on skin type. They are commonly described as “goose-bump like” in texture. Distribution is usually symmetrical, affecting:
- Upper arms (most common site)
- Thighs
- Buttocks
- Cheeks and face (especially in children and adolescents)
- Less frequently, the trunk and lower legs
1. Overall Appearance of Lesions:
The characteristic of keratosis pilaris is the formation of small, rough, keratotic papules. The papules are secondary to keratin plugging of the hair follicles. In contrast to acne, these lesions are not inflamed pustules but separate, hard, and sometimes minimally elevated bumps.
Size: The papules are usually 1–2 mm in diameter.
Shape: Dome-shaped, round, or conical.
Consistency: Coarse and hard on palpation, sometimes described as being "goosefleshed" or "sandpaper-like."
Surface: Papules can be covered with a white fine scale or possess a central keratin plug.
Plugging is in some instances so prominent that a curled hair becomes trapped beneath the surface, causing irritation or superficial erythema.
2. Distribution of Lesions:
Keratosis pilaris possesses an extremely characteristic distribution pattern, by which it can be distinguished from other follicular dermatoses.
Extensor surfaces of upper arms
Thighs (particularly outer surfaces)
Buttocks
Cheeks & occasionally the jawline (especially in children and adolescents)
Forearms, Back, Lower legs: The lesions are generally bilateral and symmetrical in their distribution, which is a helpful diagnostic point. For instance, both of the upper arms are affected to an equal extent and not one side more than the other.
3. Skin Texture:
One of the most notable characteristics of Keratosis pilaris is the surface roughness of skin. The skin is coarse & pebbly to palpation, like:
Sandpaper, Chicken skin, Plucked gooseflesh.
The texture is also usually more obvious than visible appearance. Patients complaines about the skin not being smooth, particularly when rubbed or touched, even if bumps are unobtrusive to the eye.
4. Changes in Color:
Color of keratosis pilaris lesions also varies based on a host of factors such as skin type, degree of inflammation, and chronicity.
The papules could be flesh-colored, white, or pale pink.
Some of the lesions have border erythema, giving them a red "pinpoint" appearance.
The papules could be dark brown, grayish, or hyperpigmented.
Post Inflammatory Hyperpigmentation is more prevalent.
In either case, coloration is usually mild and does not indicate significant inflammation, unlike acne or folliculitis.
5. Symmetry and Pattern:
A typical feature of Keratosis pilaris is symmetrical and bilateral distribution. Both thighs, or both cheeks, and both arms are usually involved equally. This distinguishing feature separates it from folliculitis, where lesions may occur more randomly or asymmetrically.
Distribution is folliculocentric—one papule per hair follicle orifice. Follicular involvement is one of the main diagnostic features.
6. Symptoms and Patient Complaints:
Keratosis pilaris is usually asymptomatic but, at times, produces minimal discomfort. Some of the symptoms are:
- Dryness: The skin around the follicle is dry.
- Itching (pruritus): Mild and transient; more frequent in winter or dry climate.
- Irritation: Uncommon, but may occur if papules become inflamed or the patient scratches.
- Cosmetic issue: Most frequent complaint is with the look and texture of the skin, particularly if lesions are on uncovered areas of body such as the face or arms.
Surprisingly, Keratosis pilaris is not painful and does not generate systemic symptoms.
7. Seasonal Changes:
Severity of keratosis pilaris tends to vary seasonally:
- Worsens during cold, dry weather.
- Lower humidity dries out the skin, which increases roughness.
- Winter heating systems contribute additional dryness.
- Improves during warm, humid weather
- Higher water content of the skin makes keratin plugs softer.
- Sunlight may cause transient increase in skin smoothness.
- Seasonal change is a helpful clinical hint to diagnosis.
8. Age of Onset and Natural Course:
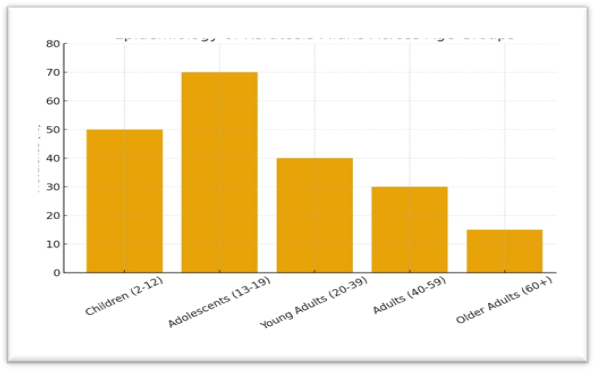
- Onset: Keratosis pilaris often begins in childhood or early adolescence.
- Peak prevalence: Late childhood to adolescence, particularly at puberty.
- Course: Most disappear with age. In others, it continues into adult life, though it becomes less severe with age. Since it is chronic and recurrent, patients have "always had bumpy skin."
9. Associated Conditions:
Keratosis pilaris also presents in association with other dermatologic conditions, most notably those of abnormal keratinization or dryness.
- Atopic dermatitis (eczema): Individuals with atopic predisposition are predisposed to Keratosis pilaris.
- Ichthyosis vulgaris: Strongly associated; both share a genetic association with mutations in filaggrin.
- Dry skin (xerosis): Keratosis pilaris is more evident in patients who have inherently dry skin.
- Other associations: Rarely associated with disorders like Down syndrome or obesity.
These are not diagnostic, but give extra clinical information.
10. Variations of Keratosis Pilaris:
Although the classic one is most prevalent, there are variations with slightly different clinical presentations:
- Keratosis pilaris rubra: Includes red or erythematous papules. Prevalently affects the face, arms, and thighs. Produces more extreme redness.
- Keratosis pilaris alba: Papules are pale or skin-colored. Less erythematous-associated.
- pilaris rubra faceii: Affects cheeks with diffuse redness and papules. May be confused with Keratosis acne or rosacea.
Keratosis pilaris atrophicans: Uncommon variant of scarring follicular atrophy. Encompasses conditions like ulerythema ophryogenes (eyebrow involvement).
Identification of these variants assists clinicians in distinguishing between subtle presentations.
11. Psychosocial Impact:
Although Keratosis pilaris is not medically significant, its effect on quality of life can be huge. Patients can feel:
Self-consciousness due to visible lesions on the arms, cheeks, or legs. Low self-esteem, particularly during adolescence. Anxiety due to the false assumption that Keratosis pilaris is an infectious or hygienic illness. Reassurance and counseling are a crucial component of clinical management.
ASSOCIATIONS WITH OTHER CONDITIONS:
Keratosis pilaris is a benign dermatologic condition cutaneous presents with numerous small, rough papules most classically scattered over the extensor surfaces of arms, thighs, buttocks & occasionally the cheeks. While it is oftentimes simply considered an unproblematic cosmetic issue, studies have determined that Keratosis pilaris is most often not an independent event. Rather, it may occur in association with a wide range of dermatologic & systemic diseases. These relationships are of interest to researchers and clinicians alike in the context that they provide information on possible common mechanisms, genetic overlaps, as well as clinical correlations. Discussion below also considers the most suitable relationships of Keratosis pilaris with special emphasis on atopic dermatitis, ichthyosis vulgaris, obesity and metabolic syndrome, and other follicular diseases.
1. Relationship with Atopic Dermatitis (AD):
- Epidemiological Evidence: A well-documented and chronic relationship between Keratosis pilaris and AD has been reported. Research has shown that AD patients are more susceptible to Keratosis pilaris, and Keratosis pilaris in AD is very prevalent in relation to the normal population. Some dermatologists have even gone ahead and referred to Keratosis pilaris as the "atopic diathesis", a cluster of clinical findings typical of atopic patients.
Shared Pathophysiological Mechanisms:
The link between Keratosis pilaris and AD can be attributed to a shared disruption in immune regulation and epidermal barrier function. Both diseases share disturbances in keratinization along with disruption of the epidermal barrier resulting in inflammation and dryness.
- Barriers Dysfunction: Filaggrin gene (FLG) and other barrier protein mutations compromise the barrier ability of skin to retain water & act as a shield against irritants in AD. Keratosis pilaris is also supposed to be a result of keratin plugging of the orifice of the follicle by abnormal keratinization. [11]
- Genetic Overlap: A few reports indicate that filaggrin mutations can not only predispose to Keratosis pilaris as well as AD and ichthyosis vulgaris but also cause Keratosis pilaris. Genetic overlap lends support to the possibility that Keratosis pilaris could be an endophenotype or clinical marker of the atopic spectrum broadened to encompass Keratosis pilaris.
- Inflammatory Environment: Th2-biased immune responses present in AD could heighten follicular plugging and papulogenesis. The xerotic milieu of AD itself further increases the visibility of Keratosis pilaris.
Clinical Implications:
AD patients are predisposed to Keratosis pilaris development during the adolescent years, with subsequent erythematous or more inflamed papules.
Erythematous or more inflamed papules are followed by atopic Keratosis pilaris, which can cause pruritus, cosmetic distress, and lower quality of life, although Keratosis pilaris is asymptomatic in non-atopic subjects.
This association is significant because treatment of Keratosis pilaris in AD patients can involve intensive moisturization, barrier repair therapy, and sometimes anti-inflammatory treatment. [12]
2. Association with Obesity and Metabolic Disorders:
- Observational Studies: Evidence over the past ten years has implicated a relationship between Keratosis pilaris and obesity and associated metabolic disorders like insulin resistance, metabolic syndrome, and dyslipidemia. Although not proven to cause, epidemiological evidence indicates that Keratosis pilaris occurs more commonly in persons with a greater body mass index (BMI).
- Possible Explanatory Mechanisms: [13]
- Skin Physiology in Obesity: The obese patient has changed skin physiology, such as enhanced sweat retention, barrier dysfunction, and microinflammation. All these changes have the potential to worsen Keratosis pilaris lesions.
- Systemic Inflammation: Obesity causes a state of chronic low-grade inflammation, which may be synergistic with the follicular inflammation of Keratosis pilaris.
- Hormonal Influences: Adipokine dysregulation and insulin resistance can influence keratinocyte growth and differentiation to create hyperfollicular plugging.
In the obese, Keratosis pilaris is more widespread and symptomatic. The association invites one to think of Keratosis pilaris not only in its cosmetic but also as a possible cutaneous marker of hidden metabolic risk. Promoting weight reduction and maintenance of metabolic health may indirectly enhance Keratosis pilaris.
PSYCHOSOCIAL IMPACT:
Keratosis pilaris is a very prevalent skin condition of small, rough papules that normally reside on the upper arms, thighs, buttocks, and occasionally face. From a health point of view, Keratosis pilaris is benign: it is not a source of much or even any physical pain, it is not a symptom of systemic illness, and it is not infectious. But beyond the surface level of its clinical appearance is a true but all too frequently overlooked factor — its psychosocial impact. The condition, while not physically incapacitating, will have a profound impact upon self-esteem and interpersonal relationship. Physical manifestation of Keratosis pilaris is a strong factor that influences self-esteem, social role, and quality of life in most patients, especially adolescents and young adult. [20]
1. The Problem of Cosmetic Noticeability:
Compared to cutaneous chronic inflammatory dermatoses like psoriasis or atopic dermatitis, Keratosis pilaris is a rare cause of burning, tenderness, or pruritus. Its most debilitating failure is not pain but cosmetic visibility. The miniature, thick, red papules render the skin sandpapery hard to the touch, an erroneous assumption that it is "acne," "rash," or "poor hygiene." It is embarrassing and socially stigmatizing.
Keratosis pilaris is also most commonly found in childhood and adolescence - years of increased self-concept, body image, and peer acceptance susceptibility. Keratosis pilaris is most commonly found in teenagers who say they feel "different" or "not perfect" from others, particularly when the papules are visible on cheeks, forearms, or legs. Social comparison, especially in today's age of social media and photoshopped ideals of beauty, increases self-consciousness.
• Avoidance of short-sleeved shirts, swimming, or activity with use of involved areas is described in the majority of adolescents.
• Avoidance of physical education class or athletics on the basis of concern over embarrassment is described in others.
• Avoidance diminishes access to social integration and threatens physical health through reduced levels of activity.
2. Comparative Insights: Keratosis pilaris and Other Dermatological Conditions:
Keratosis pilaris vs Acne:
Acne vulgaris is the most studied dermatological condition in the area of psychological morbidity. Like Keratosis pilaris, acne typically arises in adolescence and is physically apparent. Although while acne is typically marked by pain, inflammation, and scarring ability, Keratosis pilaris is not. But whereas Keratosis pilaris patients' pain is of roughly the same magnitude as that of mildly acnes patients, it is for the same reason working in both cases: physical visibility and subjective difference from normal-skin appearance.
Keratosis pilaris vs Psoriasis and Atopic Dermatitis
In contrast to psoriasis & atopic dermatitis, Keratosis pilaris is not associated with systemic inflammation or severe itching. Embarrassment and lifestyle restriction do occur, nonetheless. This difference reminds us that psychosocial morbidity of skin disease is separated from medical severity. Mild illness can have enormous emotional weight when visible skin surfaces are altered.
3. Quality of Life Studies: [19]
The psychosocial impact of Keratosis pilaris is shown by current quality of life (QOL) studies
- Low self-esteem, avoidance of social function, and resistance to physical exposure activity are described by patients.
- After some studies, Keratosis pilaris patients indicate self-image problems such as acne patients, despite the fact that Keratosis pilaris is not symptomatic.
- It highlights the discrepancy between patient report (disturbing) and clinical impression (benign).
- This discrepancy implies the necessity for standardized measures of Keratosis pilaris severity, not only for dermatological presentation (range and frequency of papules) but also for psychosocial impairment.
CURRENT TREATMENT OPTIONS:
Keratosis pilaris (Keratosis pilaris) is still one of the most frequent but frustrating dermatologic complaints seen in the clinic. Benign but frequently asymptomatic, its cosmetic presentation- follicular papules, erythema, and textural alteration-provides intense cosmetic morbidity, most typically in adolescents and young adults. Thus, they come to the clinician or the over-the-counter sector with a desire to enhance the cosmetic appearance of the skin. Even though treatment of Keratosis pilaris is normally rational, since no cure exists and relapse is an easy job once therapy has stopped. Therapeutic modalities are thus more or less symptomatic in nature and try to enhance evenness of the skin, alleviate erythema, and maximize cosmetic results.
7.1 Emollients:
Liberal moisturizing is the foundation of Keratosis pilaris treatment. Keratosis pilaris is causally linked with dryness, roughness, and barrier defect, and hence emollients play a central role in softening papules & lessening tactile roughness.
Mechanism of action: Emollients hydrate the stratum corneum, diminish transepidermal water loss & enhance skin barrier function. Mild keratolytics or humectants may be incorporated in some mixtures that facilitate desquamation of keratin plugs.
Formulations of choice: Urea creams (10–20%): Both moisturize and have keratolytic effect by disrupting hydrogen bonds in keratin. Lactic acid lotions (5–12%): Less irritable exfoliants with humectant properties, providing smoother texture. Ceramide moisturizers: Repair barrier lipids and potentially offer long-term hydration.
Clinical effects: Emollients do not eradicate lesions in most instances but obviously enhance skin feel and appearance with sustained therapy. But this must be repeated daily, because relapse is quick when it is discontinued. [21]
7.2 Topical Retinoids:
Topical retinoids such as tretinoin, adapalene, and tazarotene are reserved for resistant cases.
Mechanism of action: Retinoids re-establish differentiation of keratinocytes, decrease hyperkeratinization, and perhaps remove plugged follicles. They also improve epidermal turnover, firmness and color.
Efficacy: There have been many small trials which demonstrate improvement of roughness and pigmentation with retinoid treatment. Less irritating adapalene can be used where there is sensitive skin. [22] , [23]
7.3 Laser and Light Treatment:
In cases with an excess of cosmetic morbidity, laser and light therapy constitute a new choice. They are used mainly for the treatment of erythema and papules that are refractory to treatment.
Treats vascular elements of erythematous Keratosis pilaris. Decreases redness and inflammation, particularly beneficial in keratosis pilaris rubra.
Mechanism of action: The Pulsed Dye Laser emits an intense beam of light at a specific wavelength (commonly 585–595 nm) that targets oxyhemoglobin - the red pigment in blood vessels. This process is based on the principle of Selective Photothermolysis, which means: The laser selectively heats and destroys the target (blood vessels causing redness or inflammation) while sparing surrounding skin tissues.
- Nd: YAG (Neodymium-Doped Yttrium Aluminum Garnet) Laser:
More penetrating & can treat papules and pigmentation.
Mechanism of action: An Nd: YAG laser works by using Nd: YAG as the active medium to produce a high-intensity beam of light, primarily at a wavelength of 1.064um. A flash lamp pumps energy into the neodymium ions, exciting them to higher energy levels. These eager ions then come back to a lower energy state, releasing photons in a process called stimulated emission, which are amplified between two mirrors to create a laser beam.
Potentially improves skin texture and colour but experience is not common.
Mechanism of action: A fractional CO2 laser works by creating microscopic columns of heat and micro-ablations in the skin, which promotes the body's natural healing mechanism to generate new, healthier tissue. The laser's infrared light is absorbed by water in the skin, vaporizing the outer layers and stimulating collagen production for a firmer, smoother, and tighter appearance. The "fractional" aspect leaves healthy skin between the micro-injuries, allowing for faster healing than traditional, fully ablative lasers.
- Intense pulsed light (IPL):
Treats vessels and pigment with non-coherent light energy.
Mechanism of action: IPL, or Intense Pulsed Light, targets certain pigments (chromophores) in the skin, such as hemoglobin or melanin, using broad-spectrum light. The light is absorbed, converting to heat which destroys the target cells, leading to hair removal, reduction of pigmented or vascular lesions, or collagen stimulation.
7.4 Other Modalities:
A number of other or adjuvant therapy have been used for Keratosis pilaris, but most are weakly supported by robust clinical evidence.
Is a physical abrasion utilized to buff the skin surface. Will result in temporary change but effects are fleeting. Is a minimally invasive cosmetic technique that uses a instrument to softly exfoliate top layer of skin to extract dead skin cell and enhance texture. It is nonsurgical treatment that is performed by professional and is used to treat problems like uneven acne, skin tone, scars, fine lines, and sun damage.
Peels with a number of agents including glycolic acid, salicylic acid & trichloroacetic acid have been tried. May cause deeper exfoliation but is accompanied by a higher risk of irritation and post-inflammatory hyperpigmentation.
- New topical formulations:
Several vitamin D analogues, anti-inflammatory agents, and peptides have been described recently. Evidence is preliminary and pending confirmation.
Used very infrequently, other than syndromic or refractory Keratosis pilaris. Oral retinoids are documented in individual case reports but should not be used because of their side effect profiles.
- Patients would experience:
More objective monitoring of treatment, increasing trust in therapies. Validation of problems, as their cosmetic and psychosocial problems are addressed in a formal context. Potential for access to more specific treatments as new treatments become established.
A systematic critique of current literature in turn illustrates several key gaps that are constraining improvement in clinical care, as well as scientific understanding of Keratosis pilaris. Fulfillment of the gaps is essential to promote patient outcomes, guide evidence-based practice, and drive future research.
- Most clinical trials of treatments for Keratosis pilaris are flawed by:
Small patient numbers, typically fewer than 50. Brief follow-up periods, so safety and efficacy over the long term cannot be determined. Heterogeneous outcome measures, making studies incomparable.
CLINICAL PRESENTATION AND DIAGNOSIS:
Keratosis pilaris is a benign, chronic, & prevalent keratinization disorder presenting as small, coarse, folliculocentric papules. Benign though it is, the process frequently leads to cosmetic distress and at times to discomfort, pruritus, or secondary change such as post-inflammatory pigmentation and scarring. The clinical presentation of Keratosis pilaris is according to distribution, morphology, and severity, while diagnosis is primarily clinical but aided with dermoscopy and sometimes with histopathology.
- General Clinical Features:
The characteristic presentation of Keratosis pilaris is the formation of spiny, keratotic papules measuring approximately 1mm in diameter. The papules are usually rough to palpate and have been compared to the feeling of "gooseflesh," "chicken skin," or "sandpaper." The papules form because of follicular plugging secondary to hyperproduction of keratin, which ensnares fine, coiled, brittle vellus hair within the follicular orifice. The papules in most cases are only slightly erythematous or skin-colored, but exceptions exist depending on the type of Keratosis pilaris and level of inflammation.
Generally asymptomatic in most cases, some patients do have mild pruritus, but specifically if seen in temperate climates, or as an association with xerosis (dryness). Patients are bothered more by the cosmetic effect of lesions, and so, seek out the dermatologist. [14]
Keratosis pilaris most commonly affects hair-bearing skin surfaces, particularly those over extensor surfaces. The most common sites are:
- Upper arms – the far most common site.
- Thighs – extensor surface, and sometimes bilaterally symmetrical.
- Buttocks – may have more severe perifollicular erythema.
- Face – cheeks' sides in children and young adults.
- Trunk – chest and back involvement less frequently but sometimes reported.
The condition is rarely seen on glabrous skin (e.g., palms and soles), as the presence of follicles is a pre-requisite for papule formation.
- Subtypes of Keratosis Pilaris: [15]
Several clinical presentations of Keratosis pilaris have been described, each with distinct characteristics:
- Keratosis Pilaris Rubra (Keratosis pilaris):
Characterized by prominent perifollicular erythema along with characteristic papules. Most commonly seen on cheeks and proximal arms. The erythema is also typically persistent and cosmetically disconcerting, giving the skin a reddish or inflamed appearance. Patients will often mix up this subtype with early rosacea.
Papules are whitish or grayish in color and have little erythema. This subtype is more common in patients with lighter skin. The lesions are less noticeable but can also roughen the skin.
- Keratosis Pilaris Atrophicans (Keratosis pilaris):
A less common but clinically significant subtype. Includes follicular plugging followed by scarring and atrophy with fading of papules. It occurs with alopecia (particularly of eyebrows and scalp margins) and scarring pitting. Variants of this type include ulerythema ophryogenes (eyebrow involvement) and atrophoderma vermiculatum (honeycomb scarring). This type tends to persist into adulthood and is likely to be more of a cause of psychologic distress due to scarring and hair loss. [16]
Keratosis pilaris with hyperpigmentation – more common in darker phototypes of skin, where there is inflammation leading to post-inflammatory hyperpigmented macules around papules.
Erythromelanosis follicularis facieietcolli – erythema, hyperpigmentation, and follicular papules involving rare variant limited to face and neck.
- Associated Clinical Changes:
Although papules are the primary feature, secondary changes may follow:
- Hyperpigmentation: Especially with darker skin, scratching or prolonged inflammation may lead to brownish discoloration.
- Hypopigmentation: Hypopigmentation post-inflammatory macules may be seen in a few patients, which may be mistaken for pityriasis alba.
- Scarring: Atrophic or pitted scars in the severe or chronic form, especially keratosis pilaris atrophicans.
- Alopecia: Atrophic forms are said to report alopecia, with the involvement of scalp and eyebrows.
Keratosis pilaris may masquerade or mimic a number of dermatoses. Clinical inspection is therefore prudent. The appropriate differentials are:
- Acne vulgaris: Both have follicular plugging, but lesions of acne are large, inflamed, and may be comedonal or pustular.
- Folliculitis: Infectious folliculitis is painful, tender, and pustular, compared with the small rough papules of Keratosis pilaris.
- Atopic dermatitis: Xerosis and lichenification of the atopic skin are characteristic, though Keratosis pilaris occurs in patients with atopic diathesis.
- Ichthyosis vulgaris: Scaling is diffuse, compared with the focal involvement of Keratosis pilaris in follicular openings.
- Rosacea (erythematotelangiectatic type): Rubra keratosis pilaris may be similar to rosacea, but distribution and follicular papules distinguish them.
- Pityriasis alba: Hypopigmented post-inflammatory patches in children may simulate Keratosis pilaris, but Keratosis pilaris papules are not smooth to the touch.
DIAGNOSTIC APPROACH [30]
1. Clinical History:
History-taking will generally be sufficient to render a suggestion of Keratosis pilaris. Consider:
Age of onset: Keratosis pilaris is most commonly seen in childhood or adolescence but is occasionally persistent throughout adult life.
Family history: Familial predisposition is common; several people have affected family members.
Associated conditions: Atopy, ichthyosis vulgaris, and keratoderma are common associations.
Symptoms: Symptomatically asymptomatic in most patients, but in some cause itching, dryness, or cosmetic distress.
Exacerbating factors: Cold temperature, dry climate, and low humidity can potentially aggravate symptoms.
2. Physical Examination:
Visual and palpation inspection of the skin reveal:
Small, folliculocentric papules which can be skin-colored, erythematous, or whitish. Rough texture most evident on extensor arms and thighs. Symmetry of distribution and sparing of non-follicular areas. Secondary changes such as erythema, pigmentation, or scarring according to subtype.
3. Dermoscopy:
Dermoscopy is a useful, non-destructive diagnostic tool which enhances visibility and is able to differentiate Keratosis pilaris from associated disorders. Characteristic dermoscopic findings are:
Follicular plugs of keratin, Coiled or whorled vellus hairs in papules, Perifollicular erythema and scaling, Dermal vascular ectasia, Enlarged follicular orifices, Hyper- or hypopigmentation of follicle environs.
Dermoscopy is also an objective way of recording baseline severity and follow-up treatment response, valuable in both clinical and research settings.
4. Histopathology (Rarely Indicated):
Histopathological diagnosis is rarely required but can be required for atypical or severe lesions. Characteristics are:
Hyperkeratosis and ostia plugging of follicles, Mild perifollicular lymphocytic infiltrate, Sebaceous gland atrophy in some types, Trapped vellus hair shaft in keratin plug.
5. Patient-Reported Outcomes:
Since Keratosis pilaris is normally a cosmetic and not a symptomatic skin condition, the psychosocial impact must be assessed. Some patients are self-conscious, feel lower about themselves, or are withdrawn socially due to observable lesions if the face or the exposed skin surfaces are involved.
No widely accepted standard scoring system for Keratosis pilaris severity currently exists, but physicians typically grade on:
Number of lesions, Distribution of sites involved, Severity of erythema, Roughness of skin (texture), Scarring or pigmentation. Development of severity grading is a dermatological unmet need to have standardized instruments for.
Keratosis pilaris is an innocent condition and typically self-limiting. The lesions can improve over age in a majority of patients and recover spontaneously in adulthood. Persistence into later life does take place, however, particularly in those who present with severe varieties or with coexistent atopic conditions. Dissatisfaction with appearance remains the primary concern in most patients, thus serving to highlight the importance of sensitive clinical management.
ROLES OF ACIDS, STEROIDS:
- Acid: [24] , [25]
It is a common ingredient of many acne products because it is able to clean out the pores.
- Glycolic Acid: It weakens the connections between the surface layer of the skin, made up of dead skin cells & the dermis. This provides a peeling action that causes fewer dead skin cells & oil in the pores, resulting in cleaner skin. It is also a fairly prevalent alpha-hydroxy acid, which acts to release old & dead skin cells, revealing new skin cells. Scarring is also found to improve with the application of glycolic acid, setting it up as a promising strategy for treating keratosis pilaris.
- Salicylic Acid: It is also a widely recognized element in skin-clearing treatments & targets keratosis pilaris & other acne diseases by decreasing cohesiveness between keratinocytes. Salicylic acid has been demonstrated to give skin lightening advantages while providing no major harm to pores. It treats acne by dissolving dead skin cells that clog pores & make the skin appear better. Because salicylic acid is an oil-soluble beta-hydroxy acid, it can permeate the skin's lipid layers.
- Lactic Acid: It may also be used to treat papules. By dissolving dead skin cells, it can open clogged pores and enable deeper penetration of other treatments, such as salicylic acid. Another acid that may be thought useful in the treatment of keratosis pilaris & other acne is retinoic acid, which increases the appearance of post-inflammatory hyperpigmentation & lessens atrophic acne scarring. Azelaic acid specifically: Azelaic acid is a dicarboxylic acid that has also shown efficacy against acne. Azelaic acid, well recognized for its anti-inflammatory & antioxidant characteristics, acts either in monotherapy or combination therapy to treat post-inflammatory hyperpigmentation.
- Kinase Inhibitors:
Since kinase inhibitors block enzymes known as tyrosine kinases, they have also been shown to have an impact on keratosis pilaris and its related variations. Since tyrosine kinases aid in conveying advanced signals in cells, obstructing them limits cell division & development. The majority of alopecia's negative effects, mostly skin scarring, are caused by the kinase inhibitor nilotinib. Another noteworthy kinase inhibitor is vemurafenib, a BRAF inhibitor utilized to treat metastatic melanoma, a kind of skin cancer when cells that produce color in skin turn cancerous.
- Steroids: [26] , [27]
Steroids are among the chemicals that affect keratosis pilaris. Topical & systemic steroids immediately treat acne conditions by reducing inflammation. Based on the research included in the current review, some particular examples of steroids affecting acne issues include mometasone furoate, triamcinolone, prednisone, hydrocortisone, testosterone, methylprednisolone & clobetasol propionate.
- Genetic Acids :
Keratosis pilaris is a genetic illness; hence, some of the amino acid-producing genes may have an effect on the condition. For example, the fibrinogen alpha chain & guanine nucleotide exchange factor 1 genes encode amino acids that produce proteins that affect acne & hyperpigmentation.
The importance of concentration & dose. Acids, steroids & kinase inhibitors all have an effect on keratosis pilaris, although the kinds differ depending on the quantity and dose. Acid's intended benefits for the skin may not always be realized at low doses. This will mostly impact people with sensitive skin types. Acid concentration is also determined by type of acid employed.
The dosage of steroids & kinase inhibitors. Dosages of steroids are important to consider for medications since too much or too tiny might cause unpleasant side effects. For example, testosterone is directed in doses ranging from 1.1 to 8 nmol. According to the research, the recommended doses for hydrocortisone, triamcinolone, mometasone furoate & clobetasol propionate are 2.5%, 0.1%, and 0.05%. The daily doses of prednisone and methylprednisolone are 20mg & 6mg, respectively.
Kinase inhibitor doses are also crucial. Studies show that individuals are given either 600mg or 800mg of nilotinib.
The concentration of acids, as well as the dosages of kinase inhibitors & steroids, is critical for patients suffering from skin problems since the efficacy of skincare products is dependent on the concentration of acids in skincare routine & how it disturbs various skin types. [28] , [29]
TABLE:


 Sayali Deth*
Sayali Deth*
 Om Salunke
Om Salunke





 10.5281/zenodo.19044866
10.5281/zenodo.19044866